One by one, previous treatments are failing against a disease that kills hundreds of thousands of people every year.
By Siobhan Robbins, Southeast Asia correspondent, in Cambodia
Millions of lives will be in danger if antimalarial drug resistance spreads from Asia to Africa, doctors have warned.
About half of the world’s population is at risk of malaria, but some of the drugs used to treat it have started to fail.
Currently, artemisinin-based combination therapies (ACTs) are the gold standard of antimalarial treatment – but in 2008, a parasite resistant to artemisinin emerged in Pailin, western Cambodia.
Initially, the partner drugs in ACTs could still beat the infection. However, researchers found a strain also resistant to piperaquine (a partner drug) had started to spread in 2014.
Since then, this double-resistant parasite has moved across southeast Asia and now a triple-resistant strain has been found in northern Cambodia.
Dr James Callery from The Mahidol Oxford Tropical Medicine Research Unit (MORU) told Sky News: “Previously, when we had the resistance to chloroquine in Africa, we saw a massive upsurge in deaths and morbidity from malaria, and it was only because of the ACTs that came along that we were able to bring that down and start getting it more under control.
“We found artemisinin resistance and partner drug resistance emerged in western Cambodia and then we saw it spread across Cambodia to northeastern Thailand, southern Laos and then more recently down to south Vietnam as well.
“If we get failure from [ACTs], then we will go back to the dark days of seeing all these deaths among children, and getting to the point where we might get malaria that isn’t treatable.”
Widespread ACT drug resistance could be especially catastrophic if it took hold in Africa, where 90% of the world’s malaria cases are, so the race is on to find a solution.
Until recently, the standard antimalarial drug used in Cambodia was failing in up to 60% of cases, prompting the national malaria control program to change their medication.
This same drug is now also failing in Vietnam.

Dr Callery is one of a team of experts trialling a possible alternative: a new combination of three antimalarial treatments being tested in northern Cambodia as part of a project backed by Oxford University.
The area is a malaria hotspot, with many people infected after being bitten by malaria mosquitoes which lurk in the forests where they work.
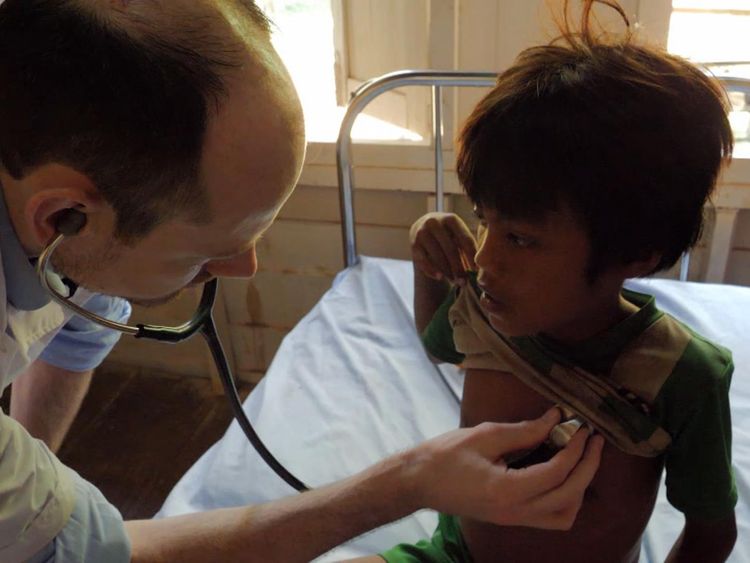
As part of a clinical trial at the MORU clinic in Siem Pang, patients are given a three-day course of three drugs.
They are monitored over six weeks to ensure the medicine has worked and they remain disease free.
Researchers say that, so far, it appears to be effective and safe.
Bun Lai, 22, developed a fever after going to cut wood and tested positive for malaria.
He said the medicine he had taken in the past did not work but he has recovered thanks to the new treatment.
“I’ve seen two or three people, including myself, having the problem of drug resistant malaria,” he said.
“I’m really worried that the children might get malaria like I did because the smaller children are not as strong as the adults.”

While southeast Asia only accounts for about 5% of the world’s malaria cases, it has a history as a breeding ground for drug-resistant strains of the parasites.

Hi I am Ashraf , I work in Paris & Institute Pasteur Cambodia . Journalist related to this study is encouraged to apply for Media fellowship about Malaria related news- see the link & terms condition
https://endmalaria.org/opportunities/rbm-partnership-end-malaria-media-fellowship?utm_content=buffer08776&utm_medium=twitter&utm_source=social&utm_campaign=general